At a Glance:
PRP is a regenerative treatment that may improve hair thickness and reduce shedding in selected individuals, particularly in early to moderate stages of pattern hair loss. It works by influencing the scalp environment rather than creating new follicles.
Results are variable and depend on diagnosis, stage, treatment consistency, and individual biology. PRP is generally approached as a management strategy requiring structured follow-up rather than a permanent solution.
PRP can support hair thickness and reduce shedding in certain types of hair loss, particularly when follicles are still active. It does not permanently restore hair in areas where follicles are no longer functioning. Outcomes depend on the diagnosis, the stage of thinning, and the consistency of treatment.
Here’s what the research says, who it works for, and what to expect.
Why People Choose PRP (And Why Some Stop It)
Interest in PRP often reflects a balance between cautious optimism and understandable hesitation. Many individuals are looking for an option that feels medically grounded yet less invasive than surgery. At the same time, uncertainty about cost, results, and long-term commitment can influence whether they begin or continue treatment.
Why People Choose PRP
For many, the decision to try PRP is driven by a desire to intervene early without committing to surgery. The appeal often lies in preserving existing hair rather than attempting to replace what has already been lost. Understanding these motivations helps clarify whether expectations align with what the treatment can realistically provide.
- Natural treatment perception: PRP uses concentrated components from a patient’s own blood, which appeals to those seeking a biologically based approach rather than synthetic medication.
- Avoiding daily medication: Some individuals prefer periodic in-clinic sessions over long-term daily topical or oral therapies, particularly when daily consistency is a concern.
- Trying PRP before transplant: PRP is often considered during early or moderate thinning as a step to stabilize hair loss before evaluating surgical options.
- Perceived safety: Because PRP is autologous, concerns about systemic side effects may be lower compared to certain pharmacologic treatments.
Why Some People Stop PRP
Discontinuation typically relates more to expectations, timing, or financial planning than to safety. Hair biology progresses gradually, and when this pace is not anticipated, confidence in treatment may decline. Evaluating these factors before starting can reduce premature withdrawal.
- Cost considerations: PRP involves an initial series of treatments followed by maintenance sessions, requiring ongoing budget planning rather than a one-time investment.
- Slow visible results: Hair growth cycles take several months. Without early visible change, some may conclude the treatment is ineffective before adequate time has passed.
- Discomfort during sessions: Mild tenderness or temporary sensitivity at injection sites can influence willingness to continue repeated sessions.
- Unrealistic expectations: Expecting complete restoration in advanced bald areas can lead to disappointment if the biological limits of follicle viability are not fully understood.
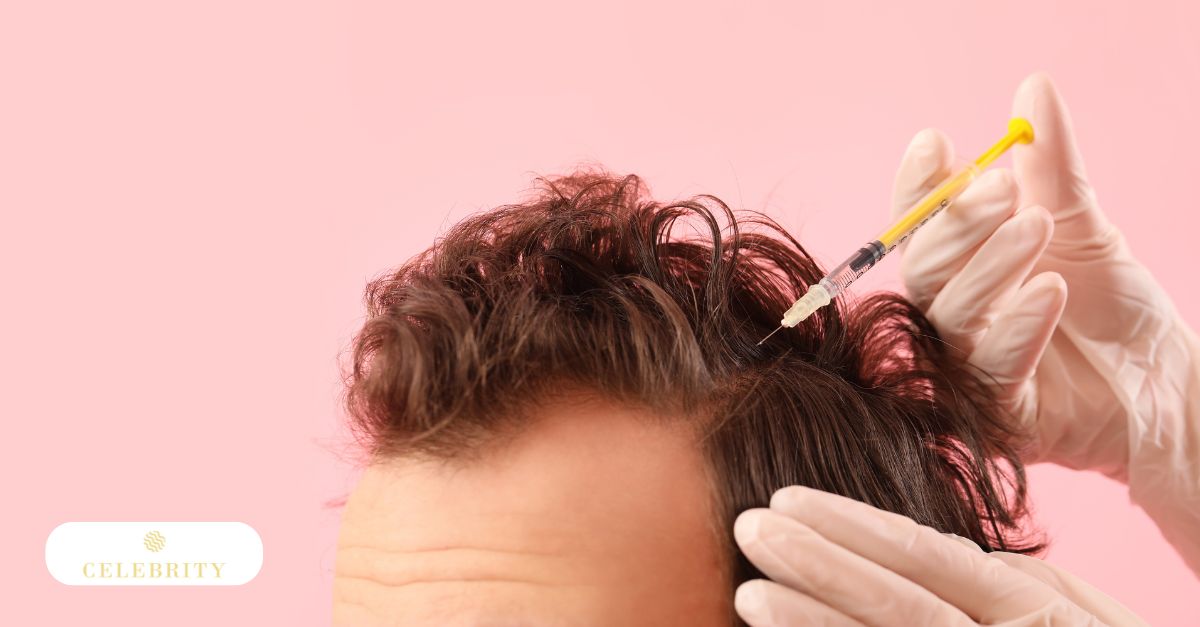
What is PRP (Platelet-Rich Plasma) for hair loss?
Platelet-Rich Plasma (PRP) is a concentrated preparation of a patient’s own blood components used in regenerative medicine. In hair restoration, it is injected into targeted areas of the scalp to support follicular activity through biological signalling rather than synthetic agents.
PRP is created through a controlled blood-processing procedure. A small sample of blood is drawn and placed into a centrifuge, which spins at high speed to separate components by density. This process isolates plasma enriched with a higher platelet concentration than normally found in circulating blood. The concentrated plasma layer is then prepared for injection.
To understand PRP, it is helpful to distinguish its components. Plasma is the liquid portion of blood, composed primarily of water, proteins, electrolytes, and signalling molecules. It functions as a transport medium for nutrients, hormones, and cellular elements. Platelets, also known as thrombocytes, are small cell fragments involved in clot formation. Beyond their role in coagulation, platelets store and release biologically active proteins known as growth factors.
Growth factors are signalling molecules that regulate cellular communication. In various tissues, they influence processes such as cell proliferation, collagen production, angiogenesis (formation of new blood vessels), and inflammatory modulation. These mechanisms are central to tissue repair following injury.
The clinical rationale for PRP in hair treatment is based on this regenerative signalling capacity. By concentrating platelets and delivering them directly into the scalp, the goal is to create a localized environment that supports tissue repair and vascular activity around existing hair follicles.
PRP is described as autologous, meaning it is derived from the same individual receiving the treatment. Because the material originates from the patient’s own blood, the risk of allergic reaction or immune rejection is considered low when proper sterile technique is followed.

How does hair growth work?
Understanding whether a treatment can influence hair loss requires a clear understanding of how hair normally grows. Hair production is a cyclical biological process regulated by cellular signalling, blood supply, and genetic factors.
Hair Follicle Structure
Each hair originates from a hair follicle, a complex mini-organ embedded in the scalp. The follicle extends from the epidermis down into the dermis and contains several key components:
- Hair bulb: The base of the follicle where active cell division occurs.
- Dermal papilla: A specialized cluster of cells at the base that regulates growth through molecular signalling.
- Matrix cells: Rapidly dividing cells that form the hair shaft.
- Sebaceous gland: Produces oil to lubricate the hair and scalp.
The dermal papilla plays a central regulatory role. It communicates with surrounding cells through growth signals and depends on an adequate blood supply to sustain follicular activity.
The Hair Growth Cycle
Hair does not grow continuously. Each follicle cycles independently through three main phases:
- Anagen (growth phase):
- This active phase can last several years. Matrix cells divide rapidly, producing the visible hair shaft.
- Catagen (transition phase):
- A brief period in which growth slows and the follicle begins to regress.
- Telogen (resting phase):
- The follicle becomes inactive, and the hair eventually sheds. A new anagen phase then begins, restarting the cycle.
At any given time, most healthy scalp follicles are in the anagen phase. Disruptions to this balance can increase shedding or shorten active growth duration.
Role of Blood Supply
Hair follicles are metabolically active structures. They require oxygen, nutrients, and signalling molecules delivered through the surrounding microvasculature. Reduced vascular support can impair cellular activity within the hair bulb and dermal papilla, influencing growth efficiency.
Role of Growth Factors
Growth factors are molecular signals that regulate cell proliferation, differentiation, and tissue maintenance. Within the follicle, these signals help maintain anagen duration and support structural integrity. Altered growth factor signalling can contribute to reduced follicular performance over time.
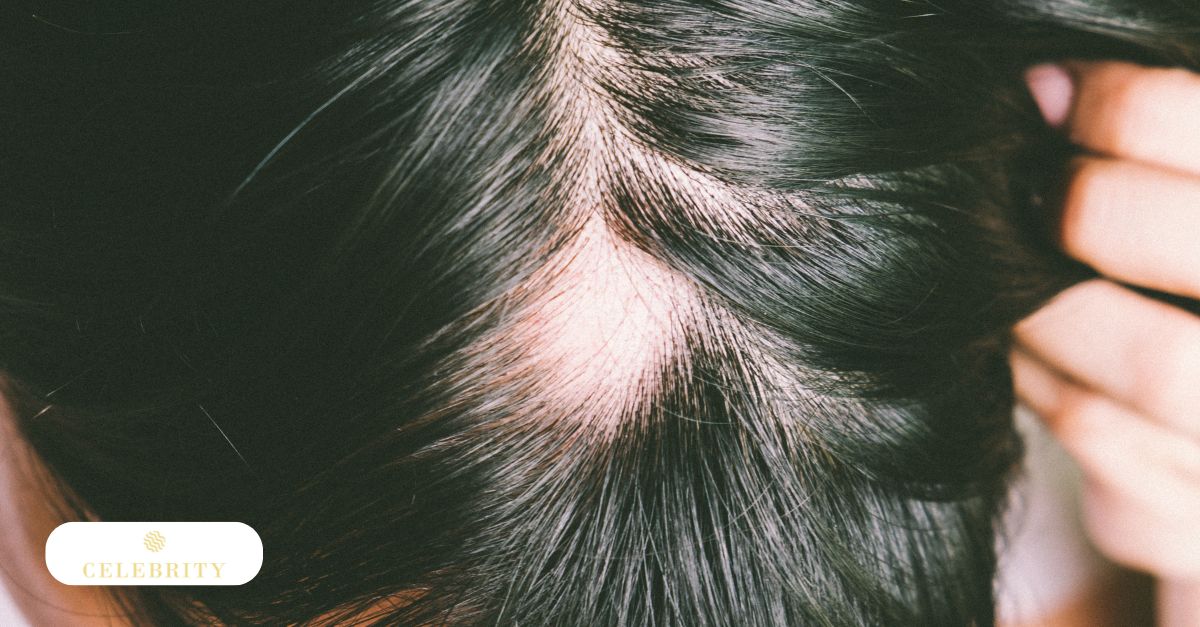
Why Follicles Shrink in Hair Loss
In certain forms of hair loss, particularly androgenetic alopecia, follicles gradually decrease in size. This process is driven by genetic and hormonal influences that alter signalling within the dermal papilla. Over successive cycles, the anagen phase shortens, and the hair shaft becomes thinner.
What “Miniaturization” Means
Miniaturization refers to the progressive reduction in follicle diameter and hair shaft thickness. Instead of producing thick terminal hairs, the follicle generates finer, shorter strands. Eventually, some follicles may produce barely visible hairs.
Importantly, miniaturized follicles are not always permanently destroyed. In earlier stages, they may remain biologically active but functionally weakened. Understanding this distinction is central to evaluating which interventions may be biologically plausible.
Why does hair loss happen?
Hair loss is not a single condition. It is a visible outcome of different biological processes that affect the hair cycle in distinct ways. Identifying the underlying cause is essential because mechanisms vary, and so does responsiveness to hair growth treatment.
Male Pattern Baldness (Androgenetic Alopecia)
This is the most common cause of progressive hair thinning in men and also occurs in women. It is driven primarily by genetic sensitivity to androgens.
Dihydrotestosterone (DHT), a derivative of testosterone, binds to androgen receptors in susceptible follicles. In genetically predisposed individuals, this interaction gradually alters follicular signalling. Over time, successive growth cycles produce thinner and shorter hairs. The process is progressive and patterned, typically affecting the hairline and crown in men and the central scalp in women.
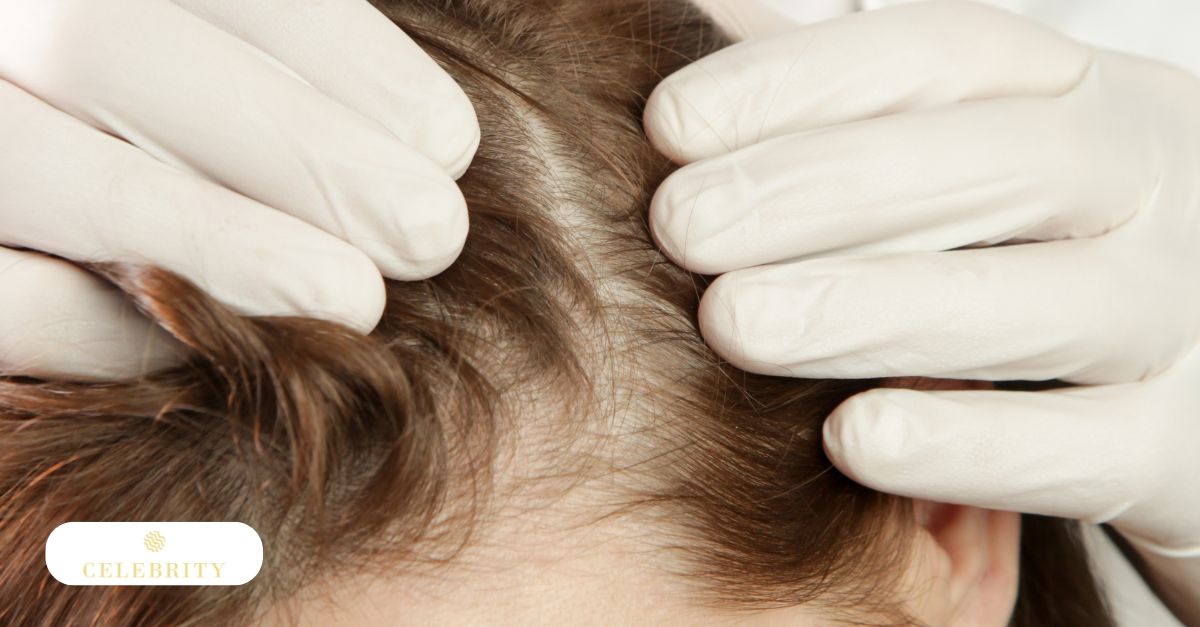
Female Pattern Hair Loss
Female pattern hair loss involves hormonal influences but presents differently from the classic male pattern. Instead of a receding hairline, women more commonly experience diffuse thinning across the central scalp.
Hormonal fluctuations, including changes in estrogen and androgen balance, influence follicular behaviour. Unlike male pattern baldness, complete bald areas are uncommon. The thinning is typically more evenly distributed, which can make early detection more subtle.
Postpartum Hair Shedding
Postpartum shedding occurs after pregnancy due to rapid hormonal shifts. During pregnancy, elevated estrogen levels prolong the growth phase of many hairs. After delivery, estrogen levels decline, and a larger-than-usual number of follicles transition into the shedding phase simultaneously.
This often results in noticeable hair shedding several months after childbirth. In most cases, the condition is temporary and stabilizes within months. However, if shedding persists beyond the expected timeframe, additional evaluation may be warranted.
Telogen Effluvium (Stress-Related)
Telogen effluvium is characterized by diffuse shedding triggered by physiological or psychological stress. Illness, surgery, significant emotional stress, or rapid weight change can disrupt the normal distribution of hair cycle phases.
A larger proportion of follicles shift into the resting phase at once, leading to increased shedding several weeks later. Unlike genetically driven thinning, telogen effluvium is typically reversible once the underlying trigger is resolved, although recovery may take several months.
Not all forms of hair loss respond in the same way to intervention. Some are progressive and genetically influenced, while others are temporary and self-limiting. Effective treatment planning depends on accurately identifying the underlying cause before selecting an approach.
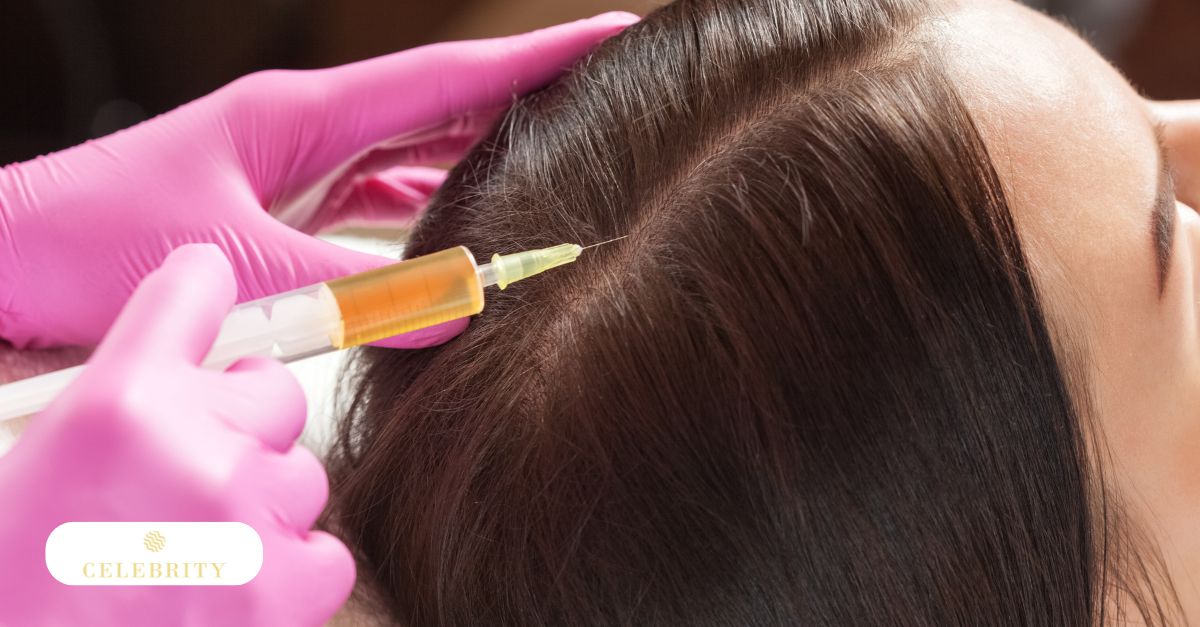
How does PRP work for hair growth?
PRP hair treatment is used to influence the scalp’s cellular environment through concentrated biological signaling. Rather than replacing lost hair, it aims to support follicles that are still structurally present but functioning below their optimal capacity.
Growth Factor Release
When platelet-rich plasma is injected into targeted areas of the scalp, platelets release stored growth factors after activation. These proteins regulate cell communication and influence processes such as cellular repair, tissue remodeling, and metabolic activity within the follicular unit.
Increased Blood Supply to Follicles
Certain platelet-derived signals are associated with angiogenesis, the development of small blood vessels. Enhanced microcirculation may improve the delivery of oxygen and nutrients to follicles, which are highly active during growth phases.
Prolonging the Anagen Phase
Hair density is partly determined by how long follicles remain in their active growth phase. Growth factor signaling may support conditions that help maintain follicles in anagen for longer durations, potentially contributing to thicker strands over time.
Stimulating Dormant but Viable Follicles
Some follicles produce progressively finer hairs yet remain biologically intact. By modifying the local signaling environment, PRP may encourage increased activity in follicles that have not permanently lost function.
Anti-Inflammatory Modulation
Low-level inflammation around follicles can disrupt normal cycling. Platelet-derived mediators are associated with regulatory effects on inflammatory pathways, which may create a more favorable environment for ongoing hair production.
Because PRP depends on existing follicular structures, its potential influence differs by stage. In earlier thinning, many follicles are present but underperforming, making biological support more plausible. In long-standing bald areas where follicles are no longer active, regenerative signaling alone may be insufficient.
In practical terms, PRP can contribute to improved thickness and reduced shedding in selected individuals, particularly when intervention occurs before extensive follicular loss. It does not recreate hair in areas where follicles have been absent for prolonged periods, and results vary based on diagnosis, timing, and treatment consistency.
What does research say about PRP for hair loss?
Clinical research on PRP for hair loss has been evaluated in multiple controlled studies, particularly in androgenetic alopecia and female pattern hair loss. Most studies measure outcomes such as hair density, thickness, and shedding patterns after a structured series of treatments.
In androgenetic alopecia, controlled trials frequently report measurable increases in hair density compared to baseline or placebo-treated areas. These outcomes are typically assessed using dermoscopy or standardized imaging. Similar findings have been observed in female pattern hair loss, although diffuse thinning patterns and hormonal variability make direct comparison across populations more complex.
PRP has also been studied both as a standalone treatment and as an adjunct to established therapies or hair transplantation. When used in combination, some studies suggest additive benefits, though isolating the independent contribution of PRP becomes more difficult in multi-modality protocols.
Across the literature, measurable improvements in follicular counts and hair thickness are reported in selected patients. However, results vary due to differences in platelet concentration, preparation systems, injection technique, session frequency, and patient selection. The absence of standardized protocols limits direct comparison between studies and makes it difficult to define uniform outcome expectations.
Evidence is stronger in early to moderate androgenetic hair loss, where follicles remain structurally present. Long-term durability, optimal dosing schedules, and comparative effectiveness against other treatments remain areas of ongoing investigation. Study conditions are also more controlled than typical clinical settings, and real-world results may reflect greater variability.
What is the success rate of PRP for hair loss?
Success rates vary based on diagnosis and stage. Studies often show measurable improvement in hair density and thickness in early to moderate androgenetic alopecia, while results are less consistent in advanced hair loss or inactive follicles.1 2
Who is a good candidate for PRP hair treatment?
Evaluating candidacy for PRP goes beyond spotting thinning. It involves assessing diagnosis, progression rate, scalp health, medical history, and past treatment responses. Baseline documentation also aids in monitoring over time.
Individuals in the earlier phases of androgen-related thinning are often considered appropriate candidates, particularly when hair density has decreased, but patterned loss remains moderate. Both men and women may fall into this category after confirmation of the underlying diagnosis.
PRP may also be appropriate for those seeking an in-clinic procedure rather than daily medication, or for individuals who prefer to explore non-surgical options before considering transplantation. In these cases, expectation alignment is essential. The goal is typically stabilization and measurable improvement in thickness rather than dramatic restoration.
Clinical screening identifies cases where PRP treatment may be unsuitable. Areas with long-term hair loss are unlikely to respond, and patients with blood disorders, platelet dysfunction, scalp infections, uncontrolled systemic diseases, or those on certain medications may need further medical evaluation before treatment.
What results timeline should you expect?
Hair response to PRP follows biological timing rather than immediate visual change. Because hair cycles and tissue remodeling occur gradually, visible improvement develops over months rather than days. Understanding this progression helps set appropriate expectations.
Immediately After Treatment
The first phase reflects procedural effects rather than hair growth changes.
- Mild swelling at injection sites
- Temporary tenderness or scalp sensitivity
- Possible short-term increase in shedding
Temporary shedding, when it occurs, does not indicate treatment failure. It reflects a shift in hair cycling that may precede stabilization.
1–3 Months
Early changes tend to be subtle and often noticed more in shedding patterns than density.
- Reduced daily hair shedding
- Early signs of thicker hair strands in some areas
At this stage, improvement is typically gradual. Many individuals observe decreased hair fall before visible fullness becomes apparent.
3–6 Months
More measurable changes may become noticeable during this period.
- Improvement in overall density in treated areas
- Visible change in hair texture or strand thickness
Progress during this phase may include fuller appearance in thinning zones and slowing of progression. Results continue to depend on individual response and consistency of the treatment schedule.
How long do PRP results last?
PRP (Platelet-Rich Plasma) therapy does not provide a permanent solution to pattern-related hair loss. Its effects require ongoing management, as improvements can diminish over time without further sessions. Maintenance treatments are recommended to support follicular health, with the frequency determined by clinical assessment rather than a fixed schedule.
Genetic predisposition continues to influence hair characteristics even after treatment. Individuals with strong hereditary patterns of thinning may require more consistent follow-up to maintain stability. Conversely, those with slower progression may observe longer intervals between sessions.
Lifestyle factors can also affect durability. Nutritional status, stress levels, hormonal changes, and overall scalp health influence how hair behaves over time. These variables do not negate treatment effects, but they can affect how long visible improvements are sustained.
In practical terms, PRP is generally approached as a management strategy rather than a one-time correction. Ongoing evaluation allows treatment intervals to be adjusted according to individual response and progression patterns.
How many PRP sessions are needed?
PRP for hair loss is typically delivered as a structured treatment plan rather than a single session. The number of sessions depends on diagnosis, severity, and individual response observed during follow-up assessments.
Most protocols start with an induction phase that includes several sessions spaced weeks apart. This phase aims to create a consistent biological stimulus for the scalp, as hair follicles respond gradually and benefit from cumulative exposure.
After this phase, patients move into maintenance sessions scheduled at longer intervals to sustain improvements and manage ongoing progression. The timing of these sessions varies based on individual responses.
Visible changes typically appear after the initial series rather than after the first appointment. Since hair production is slow, multiple sessions are necessary to align with natural growth cycles.
Financially, PRP should be treated as a phased treatment plan, with costs associated with both the initial series and ongoing maintenance. Planning helps facilitate informed decision-making and reduces the chance of discontinuation before meaningful results are seen.
Is PRP for hair loss safe?
PRP hair injections are generally considered a low-risk procedure when performed in an appropriate clinical setting. Because it uses the patient’s own blood components, the likelihood of allergic reaction or immune rejection is low compared to treatments involving synthetic substances.
Most side effects are mild and temporary. These may include localized swelling at injection sites, scalp tenderness, and short-term sensitivity. Serious complications are uncommon when proper technique is followed.
Safety also depends on how the procedure is performed. Sterile processing of the blood sample, correct preparation methods, and appropriate injection technique are essential to reduce infection risk and ensure consistent application. Treatment should be administered by a trained medical provider familiar with scalp anatomy and injection protocols.
A consultation with our team at Celebrity Laser & Skin Care helps identify contraindications such as platelet disorders, active scalp infections, or medical conditions that may affect healing.
PRP vs Other Hair Loss Treatments
Hair loss treatments differ in how they influence follicles, how they are delivered, and what level of commitment they require. Comparing these options helps clarify where PRP fits within a broader management plan.
PRP vs Minoxidil
Minoxidil is a topical medication applied daily to the scalp. Its primary mechanism involves vasodilation and local stimulation of hair follicles. It requires ongoing daily use to maintain effects.
PRP, by contrast, is administered in-clinic through periodic injections. Rather than daily chemical stimulation, it relies on concentrated biological signaling delivered at defined intervals.
Minoxidil is non-invasive and generally lower in cost over short periods, but requires long-term adherence. PRP involves procedural visits and higher upfront session costs, structured into phases rather than daily application.
PRP vs Finasteride
Finasteride is an oral prescription medication that reduces conversion of testosterone to dihydrotestosterone (DHT), targeting a hormonal driver of pattern hair loss.
PRP does not alter systemic hormone levels. Instead, it focuses on local scalp signaling. Finasteride can be effective in slowing progression in androgen-related hair loss but carries potential systemic side effects that require medical discussion.
Cost structures also differ. Finasteride is typically a recurring medication expense, while PRP involves staged in-clinic sessions with maintenance over time.
PRP vs Hair Transplant
Hair transplantation is a surgical procedure that relocates follicles from donor areas to thinning zones. It is invasive and typically performed once or in a limited number of sessions.
PRP is minimally invasive and does not move follicles. It aims to support existing hair rather than create new distribution patterns. Transplant procedures generally involve higher single-procedure costs, while PRP is structured as a series of treatments.
In some cases, PRP may be used adjunctively after transplantation to support graft recovery. However, it does not replace surgical redistribution when follicles are absent.
Combination Therapy: PRP and Microneedling
Microneedling creates controlled micro-injuries in the scalp to stimulate repair pathways. When combined with PRP, the microchannels may facilitate the distribution of platelet-derived factors within treated areas.
Combination therapy may be considered when a clinician determines that additional stimulation could complement PRP alone. Suitability depends on scalp condition, tolerance for procedural intensity, and overall treatment goals.
| Treatment | Mechanism Focus | Delivery Method | Invasiveness | Cost Structure | Maintenance Required |
| PRP | Local Growth Factor Signalling | In-Clinic Injections | Minimally Invasive | Session-Based Treatment | Yes |
| Minoxidil | Topical Vasodilation and Stimulation | Daily Topical Use | Non-Invasive | Ongoing Product Purchase | Yes |
| Finasteride | Systemic DHT Reduction | Daily Oral Medication | Non-Invasive | Ongoing Prescription Cost | Yes |
| Hair Transplant | Surgical Follicle Relocation | Surgical Procedure | Invasive | Higher One-Time Cost | Limited Follow-Up |
| PRP + Microneedling | Combined Signaling and Repair Stimulus | In-Clinic Procedure | Minimally Invasive | Session-Based Treatment | Yes |
Each option differs in mechanism, commitment level, and financial structure. Selection depends on diagnosis, progression pattern, tolerance for maintenance, and clinical evaluation rather than a single preferred approach.
How to Track Progress Properly
Hair changes occur gradually, and perception alone can be misleading. Without structured tracking, individuals may discontinue treatment before a meaningful evaluation is possible. Objective monitoring provides clearer insight into whether a treatment plan should be continued.
Monthly photographs in consistent lighting
Standardized photos taken from the same angles and under similar lighting conditions help document subtle changes in density or texture. Variations in lighting or styling can create false impressions of improvement or decline.
Shedding tracking
Monitoring changes in daily shedding patterns can provide early indicators of stabilization. This may include observing hair in the shower drain or during brushing, rather than relying solely on memory.
Professional follow-ups
Periodic in-clinic assessments allow for dermoscopic comparison, density evaluation, and documentation of measurable changes. Clinical review reduces reliance on subjective interpretation.
When to reassess
Reevaluation is typically appropriate after completion of an initial treatment phase. If no measurable change is observed within a reasonable timeframe, adjusting the plan or exploring alternative strategies may be considered.
A structured tracking approach supports realistic expectations and helps reduce uncertainty around treatment decisions.

PRP Hair Treatment in North Vancouver – What to Consider
When considering PRP for hair loss, clinical standards and provider expertise significantly influence consistency and safety. Preparation methods, injection technique, and diagnostic accuracy all affect how appropriately the treatment is delivered.
Provider experience is important. A proper consultation should confirm the diagnosis, review medical history, and clarify realistic expectations before recommending PRP. Centrifugation systems and platelet preparation protocols can differ between clinics, making quality control and sterile processing essential.
Treatment plans should be individualized. Session timing, total number of treatments, and follow-up schedules are best determined through assessment rather than a uniform template. Medical supervision also allows appropriate screening for conditions that may affect healing or response.
In North Vancouver, Celebrity Laser & Skin Care provides PRP within its hair growth and restoration services. The clinic follows a consultation-based approach, with personalized assessment guiding treatment planning.
To determine whether PRP is appropriate for your situation, schedule a consultation to assess your hair loss pattern and review your treatment options with a qualified provider.